In health and wellness circles, the phrase “blood biomarker tracking” is everywhere. From quantified-self enthusiasts and biohackers to clinicians and longevity researchers, it’s becoming a shorthand for “smart, data-driven health decisions.” But beneath the hype lies a more nuanced reality: is all this tracking truly worth the cost—financially, mentally, and medically? Let’s break it down.
What Are Blood Biomarkers, Really?
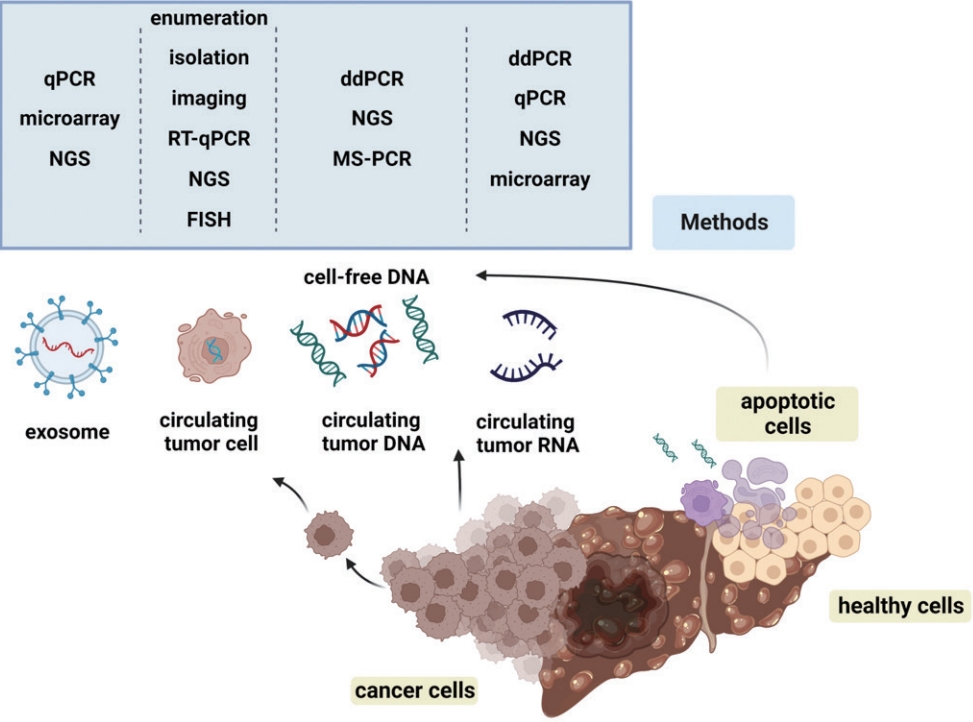
At its core, a biomarker (short for biological marker) is any measurable indicator of a biological state or condition. This can include molecular signals in blood, urine, or tissue that reflect physiological processes. Blood biomarkers include glucose, cholesterol, inflammatory proteins like CRP, hormones, and even fragments of DNA floating in plasma like cell-free DNA (cfDNA) used in liquid biopsies.
Why does this matter? Because blood circulates through every organ system. A single drop of blood can reveal something about metabolic health, immune response, organ function, and even cancer progression. Biomedical science has advanced rapidly, enabling detection of increasingly subtle signals that were invisible a decade ago.
Yet, this sophistication brings complexity: how should we value that information? Is knowing more always better? That’s where cost vs benefit becomes critical.
The Promise: Why Blood Biomarker Tracking Seems Attractive
Here are the most compelling reasons individuals and clinicians are flocking to track biomarkers:
1. Personalized Health Intelligence
Instead of inferring health from general symptoms, biomarkers provide objective data. They reveal hidden trends—such as rising blood sugar weeks before a diabetes diagnosis or subtle inflammation linked to cardiovascular risk.
Digital health companies and platforms now use AI to interpret these inputs, turning raw data into actionable insights like diet adjustments or exercise regimens.
2. Early Detection and Prevention
One of the biggest promises of biomarker monitoring is catching disease before symptoms appear. For example, in the context of Alzheimer’s disease, blood biomarkers can streamline diagnosis and reduce reliance on costlier tests like PET scans or spinal fluid analysis.
When health problems are identified early, interventions—whether lifestyle shifts or medications—can reduce long-term cost and suffering.
3. Tailored Optimization of Health and Performance
Athletes and biohackers often use biomarkers to fine-tune nutrition, training loads, and recovery. Knowing one’s lactate levels or cortisol rhythm can mean the difference between peak performance and overtraining. Beyond athletes, regular folks can also benefit from metabolic optimization insights that tailor lifestyles to individual biology.
4. Data-Driven Clinical Decisions
For health professionals, biomarkers lead to more informed decisions. In oncology, for example, specific markers help determine which therapy may work best, and can indicate whether treatment is succeeding or failing—saving time, money, and suffering associated with ineffective regimens.

The Other Side: Costs, Limits, and Drawbacks
Despite this promise, the answer to “Is it worth it?” isn’t a simple yes/no. Tracking biomarkers carries real limitations and costs that deserve scrutiny.
1. Financial Cost Doesn’t Always Scale With Value
Not all biomarker tracking is expensive, but the most detailed panels often are. A basic lab profile might be inexpensive, but comprehensive tests covering dozens or hundreds of markers—especially when paired with interpretative AI dashboards or clinician review—can run hundreds to thousands of dollars annually.
For example, a newer health panel service tied to a wearable device may provide insights for a relatively modest $99 per year, but the depth and actionability of data vary.
Thus, paying for lots of data doesn’t necessarily equate to better or more useful health outcomes.
2. Actionability Gap
Having data isn’t the same as knowing what to do with it. A very common complaint from users of advanced health dashboards is that the recommendations—whether AI-generated or clinician-offered—often boil down to generic advice: “eat better”, “sleep more”, “exercise”. While valuable, these suggestions can feel disappointingly universal.
Actionability becomes even murkier when tracking is done outside clinical oversight, where individuals may misinterpret trends and take inappropriate actions.
3. Psychological and Behavioral Costs
Tracking health metrics can lead to anxiety and obsession. A phenomenon known as data fixation arises when individuals obsess over small fluctuations that have little clinical significance. This can reduce quality of life without offering measurable health improvements.
4. The False Precision Trap
Biomarkers can be affected by diet, stress, hydration, time of day, and even how blood is drawn. Interpreting small changes as meaningful trends without understanding natural variability is a common mistake.
Moreover, correlation does not always imply causation: a high CRP level might reflect an infection, chronic inflammation, or even recent exercise—depending on context. Responsible interpretation requires nuance that technology alone can’t always provide.
Wearables and Non-Invasive Alternatives
The landscape is changing. Traditional blood draws are invasive, inconvenient, and sometimes costly. Emerging technologies are reducing these frictions.
Cutting-edge non-invasive sensors aim to track biomarkers through sweat, skin, or interstitial fluid without needles. For example, research in Singapore has developed wearable sensors capable of monitoring cholesterol and lactate through the skin, potentially eliminating frequent blood draws while delivering near-real-time data.
Similarly, advances in wearable chemical sensors and digital health tools are expanding the range of continuously monitored biomarkers, lowering the barrier to frequent data collection.
These innovations promise to shift the cost-benefit balance more favorably—especially for everyday health monitoring and chronic disease management.
Cost vs Value: A Framework for Your Decision
When evaluating whether blood biomarker tracking is worth it, consider the following practical framework:
1. Define Your Goals
Are you curious about your health? Trying to manage a clinical condition? Age-optimizing? Each goal carries a different threshold for what counts as worth it.
For clinical conditions, data can be invaluable. For curiosity, it may be less so.
2. Start With Essentials
Baseline panels covering key markers like lipids, glucose, liver and kidney markers, and basic inflammation are often affordable and clinically useful.
Add specialized tests only if there is a clear clinical reason or if advised by a professional.
3. Pair Data With Action
Data without guidance is just noise. Ideally, biomarker tracking should include evidence-based recommendations or clinician input so that numbers translate into meaningful health improvements.
4. Beware of Overtracking
More data isn’t always better. Track what you will use. Avoid metrics that don’t inform decisions or lead to improvements you can realistically make.
Where the Future Is Headed
The market for blood biomarkers and related technologies is poised for explosive growth. Analysts expect dramatic increases in digital biomarker adoption, driven by remote patient monitoring, personalized medicine, and healthcare system modernization.
Coupled with AI, wearable biosensors, and enhanced analytics, future biomarker tracking could become far more predictive, preventive, and personalized than today’s snapshot-based models.
Imagine a health ecosystem where your wearable continuously reads key biochemical signals and alerts you—and your clinician—only when a meaningful shift occurs. That future is coming faster than most realize.
Final Verdict: Is It Worth the Cost?
Yes—but conditionally.
Blood biomarker tracking can be transformative when aligned with clear health goals, interpreted responsibly, and integrated into actionable care strategies. For clinical monitoring, chronic disease management, and data-driven optimization, it can be worth every penny.
However, for casual curiosity or unfocused data collection, it can be expensive, anxiety-provoking, and low yield.
In short, value arises not from data itself, but from how we use it.
