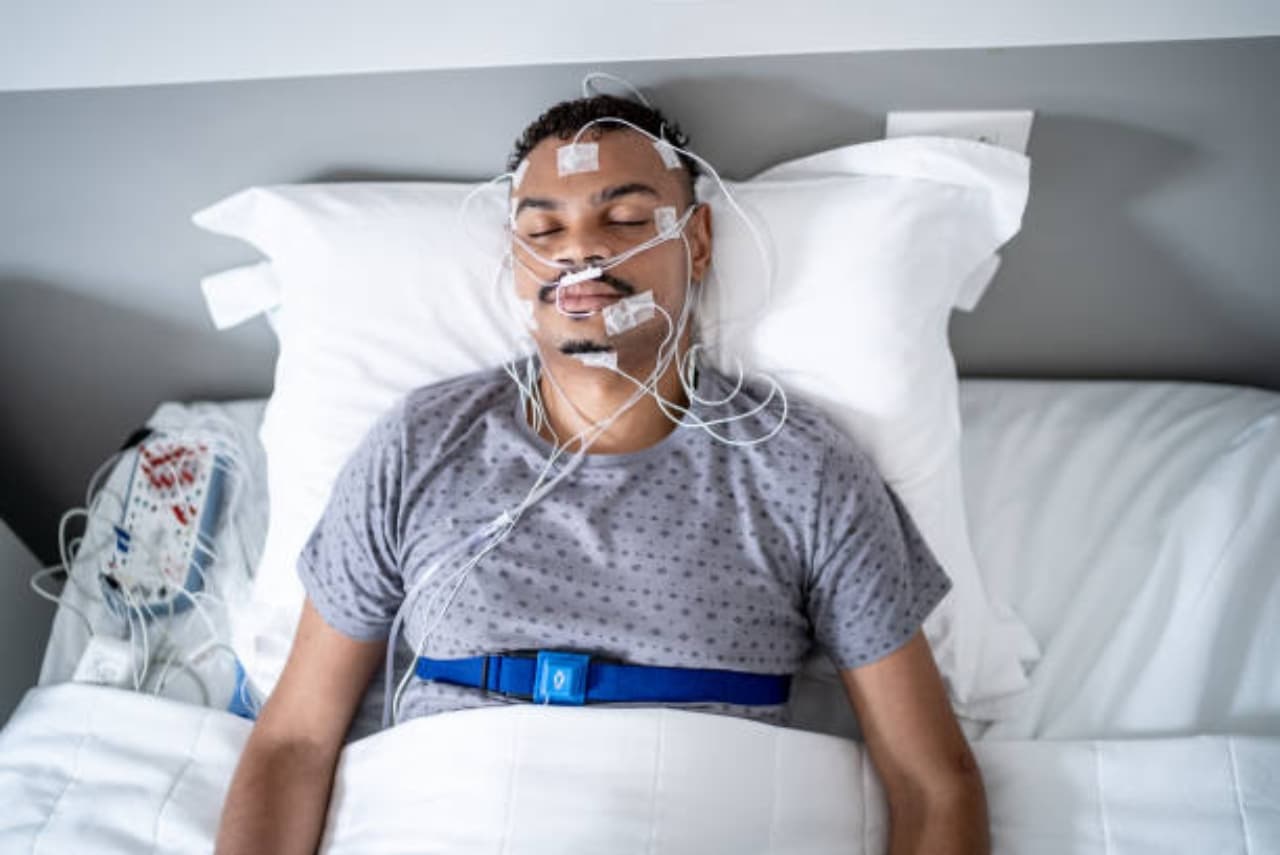
Sleep: it’s more than just “lights out.” Beneath the calm surface of closed eyes lies a dynamic biological symphony — oscillating neural patterns, cardiac rhythms, breathing cycles, hormonal pulses, and metabolic shifts. For decades, scientists used cumbersome and expensive polysomnography (PSG) in clinical labs — with electrodes glued to the scalp, chest, and face — to understand sleep’s complex architecture. But in recent years, the rise of consumer wearables like smartwatches, rings, and chest straps has promised something bold: the ability to decode your sleep biology right from your wrist or finger. But can these sleek gadgets truly tap into the intimate physiology of sleep?
In this deep dive, we will explore how wearables work, what they actually measure, where they fall short, and where they might be heading as both research tools and personal health companions.
The Science of Sleep: More Than Just Rest
Sleep is a biologically active state comprising alternating stages — from light sleep to deep (slow‑wave) sleep and rapid eye movement (REM) sleep — each with distinct physiological roles. Deep sleep supports restorative physical processes, while REM sleep is tightly linked to memory consolidation, emotional regulation, and neural plasticity. Traditionally, identifying these stages requires measuring electrical brain activity (EEG), eye movements (EOG), and muscle tone (EMG) — data only obtainable with PSG. That’s the gold standard against which everything else is judged.
But wearables don’t measure EEG or EOG — at least not yet. So the question becomes: can indirect signals serve as meaningful biological proxies for these deep internal processes?
What Wearables Can Measure
Consumer wearables typically rely on a suite of sensors that capture what external or peripheral signals they can:
- Actigraphy: Simplified motion tracking via accelerometers, commonly used to infer movement vs. stillness.
- Heart Rate & Heart Rate Variability (HRV): Photoplethysmography (PPG) sensors measure blood volume changes, giving insight into cardiac rhythm shifts during different sleep stages.
- Blood Oxygen Saturation (SpO₂): Helpful for detecting breathing irregularities associated with sleep‑related disorders.
- Skin Temperature: Minor variations are associated with circadian rhythm changes.
- Derived Metrics: Proprietary algorithms process combinations of these signals and generate sleep scores, stage estimates, and sleep quality indexes.
These tools shine at estimating sleep vs. wake states, total sleep time (TST), bedtime consistency, and broad circadian trends. Most consumer devices show good alignment (>85–90% agreement) with lab measures for distinguishing overall sleep and wake periods.
But sleep isn’t a binary phenomenon.
Sleep Stages: A Tricky Target
Where wearables truly struggle is in identifying specific sleep stages — especially distinguishing light sleep from deep or REM sleep. Unlike PSG that directly measures neural activity, consumer devices make educated guesses based on heart rate and movement patterns that correlate with sleep stages but do not capture the core physiological signals themselves.
Scientific evaluations paint a mixed picture:
- Stage classification accuracy for many devices ranges between ~50% and 75%, meaning their stage estimates are trends rather than precise measurements.
- Even leading devices show substantial variability depending on individual physiology and sleep patterns. Algorithms trained on one population may not generalize well to others.
- Motionless wake periods can easily be misclassified as sleep, and certain stages with minimal movement may masquerade as others.
This is why many experts caution that wearables are not diagnostic sleep tools, and stage percentages should be interpreted with care.
Why Wearable Sleep Data Isn’t Fully “Biological”
Even when wearables track heart rate or HRV, these are indirect proxies. They reflect autonomic nervous system activity correlated with sleep phases, but they do not capture the true electrophysiological signatures of sleep architecture like EEG does. This is a key limitation — and one that technology has not yet overcome.
Consider this: true identification of REM sleep requires tracking the electrical signals of brain activity, especially in regions associated with dreaming and muscle atonia. Wearables do not measure these directly — they infer states based on patterns that tend to accompany them. This is why two wearables can produce different stage breakdowns for the same person on the same night.
The Role of Algorithms: Magic or Mirage?
Behind every sleep metric lies a proprietary algorithm — often closely guarded, opaque, and evolving. These models rely on machine learning techniques trained on datasets that are not always publicly disclosed, validated, or representative of all users.

This creates several challenges:
- Variations in algorithm performance across demographics (age, gender, skin tone, physiology).
- Changes to algorithms that shift data interpretation without user awareness.
- Divergence between devices due to different training datasets and validation practices.
In essence, sleep scores are as much a reflection of a company’s modeling choices as they are of your biology.
Wearables and Sleep Disorders: The Clinical Frontier
Despite limitations in sleep staging, newer research has shown that wearables — especially when combined with artificial intelligence — can screen for certain sleep disorders. For example, wrist‑worn sensors that capture pulse, motion, and SpO₂ can help detect signs of sleep apnea — a condition associated with dangerous breathing interruptions.
Similarly, longitudinal sleep data, when correlated with health outcomes like cardiovascular risk or biological aging profiles, can provide valuable insights that go beyond nightly sleep scores. Indeed, large datasets from wearables have enabled researchers to identify sleep–health links not easily measurable through self‑reports alone.
Thus, while not diagnostic tools, wearables can act as scalable screening and monitoring platforms — especially for behaviors and conditions that manifest over time, rather than in isolated nights.
Toward the Future: Bridging the Gap
If wearables are to truly decode sleep biology, several technological advances are needed:
- Direct Neural Measures in Comfort: Emerging research on wearable EEG sensors embedded in fabrics or headbands suggests viable pathways for real‑world neural tracking outside the lab.
- AI Integrated with Multimodal Signals: Combining heart, motion, respiratory, and potentially neural data with advanced deep learning could elevate stage detection and reduce false classifications.
- Personalized Models: Algorithms that adapt to individual biology and circadian rhythms could outperform one‑size‑fits‑all approaches.
- Open Scientific Standards: Transparent validation against gold‑standard measures in diverse populations could build trust and accuracy.
Wearables will likely never fully replace clinical sleep studies — but they might come much closer at providing meaningful biological insights in the real world.
Practical Takeaways for Users
If you wear a sleep tracker or are considering one:
- Use it to identify patterns over time rather than obsessing over nightly details.
- Treat sleep stage labels as useful trends, not absolutes.
- Pair wearable insights with lifestyle practices like sleep diaries, consistent schedules, and professional guidance when needed.
- Recognize that wearables excel at aggregate behavior tracking — and are gradually improving but not yet equivalent to lab‑based physiology.
In short, wearables bring accessible sleep insights to millions. They don’t yet fully decode the complex neurobiology of sleep — but they are illuminating it in meaningful, practical ways.
